Ulnar Neuropathy: Small Finger Numbness and Treatment | Guide | Artur Soczka, MD, PhD
Numbness in the little finger and a weaker grip may mean ulnar nerve compression. Learn the difference between cubital tunnel syndrome and Guyon's canal syndrome.
Author: Artur Soczka, MD, PhD
Published: 2026-03-02 • Updated: 2026-04-08

Artur Soczka, MD, PhD
Orthopaedic Surgeon, Hand Surgery
He focuses on hand surgery and helps with diagnosis and treatment of hand, elbow, and shoulder pain.
View full doctor profileTable of contents
Table of contents
- Introduction: what patients should know first
- Anatomy and basic understanding
- Causes: why this condition develops
- Risk factors: who is more vulnerable
- Symptoms: typical pattern over time
- Red flag symptoms: when urgent review is needed
- Diagnosis: how clinicians confirm the problem
- Treatment options: conservative and procedural pathways
- Recovery and prognosis: realistic expectations
- Prevention and lifestyle strategies
- Patient action plan: what to do step by step
Introduction: what patients should know first
Ulnar Neuropathy is a common reason for pain, reduced hand function, and concern in everyday life. Symptoms may start gradually or appear after overload or injury. Many patients postpone evaluation, hoping the problem will settle on its own.
Numbness in the little finger and a weaker grip may mean ulnar nerve compression. Learn the difference between cubital tunnel syndrome and Guyon's canal syndrome.
This guide explains the key clinical points in plain language: typical causes, common and urgent symptoms, diagnostic pathway, treatment options, and realistic recovery expectations. The information is educational and does not replace individual medical advice.
Anatomy and basic understanding
The structures in the upper limb work together during almost every hand movement: bones, ligaments, tendons, muscles, and nerves. Even a small disturbance in this system can cause pain, weakness, reduced precision, or movement limitation.
In conditions such as ulnar neuropathy, symptoms usually develop when tissue load exceeds recovery capacity, or when injury and inflammation alter local mechanics.
Understanding this foundation helps patients interpret symptoms earlier and seek focused assessment before dysfunction becomes more persistent.
Causes: why this condition develops
In most cases, symptoms have more than one cause. Repetitive loading, static posture, forceful grip, microtrauma, and insufficient recovery can all contribute.
Some patients report clear trauma, while others develop symptoms progressively over months. Work pattern, sport technique, and daily habits often influence symptom intensity.
A key diagnostic step is separating this condition from other disorders with similar presentation, so treatment targets the actual source of pain and dysfunction.
Risk factors: who is more vulnerable
Risk is higher in people with repetitive hand-intensive work, prolonged computer use without breaks, or high-load manual tasks. Sports with repetitive upper-limb loading may also increase risk.
Comorbidities, age, prior injury, and individual anatomy can modify susceptibility and recovery speed. In many patients, symptoms fluctuate with workload and improve when load is adjusted.
Risk factors are not a diagnosis, but they support earlier evaluation when symptoms recur or start affecting daily function.
Symptoms: typical pattern over time
Most patients describe pain, local tenderness, or overload sensation triggered by specific movements. Reduced hand efficiency is common, especially during grip, fine motor tasks, and repetitive activities.
As symptoms progress, episodes become more frequent and recovery after activity may take longer. Some patients also notice stiffness, weakness, or symptom spread to nearby areas.
A structured symptom history—onset, pattern, triggers, and relieving factors—is essential for accurate clinical reasoning.
Red flag symptoms: when urgent review is needed
Prompt medical assessment is recommended if there is sudden functional decline, marked weakness, persistent numbness, progressive range-of-motion loss, or pain that does not settle despite offloading.
After trauma, warning features include increasing swelling, deformity, inability to actively move a finger or wrist, and persistent night symptoms.
Early specialist review in these situations lowers the risk of long-term deficits and helps avoid delayed treatment of significant structural injury.
Diagnosis: how clinicians confirm the problem
Diagnosis combines clinical history, focused physical examination, and selected imaging or neurophysiology tests. Examination assesses pain behavior, movement quality, strength, stability, and neurovascular status.
Depending on findings, ultrasound or X-ray is often used first, with MRI or CT in selected complex cases. When nerve involvement is suspected, EMG/nerve conduction studies may be useful.
The goal is to define both diagnosis and severity, then choose the most appropriate treatment sequence.
Treatment options: conservative and procedural pathways
Initial treatment is often conservative: load modification, ergonomic changes, guided physiotherapy, staged exercise progression, and medication where indicated.
In selected cases, ultrasound-guided injection can support symptom control. If symptoms persist despite adequate conservative management, or if function keeps declining, procedural treatment is discussed.
Procedure decisions are individualized and based on symptom duration, functional impact, examination findings, and test results.
Recovery and prognosis: realistic expectations
Outcomes are generally favorable when diagnosis is timely and treatment is matched to the stage of disease. With conservative care, improvement is often gradual and should be monitored.
After procedures, return to normal activities depends on pathology severity, tissue status, and job demands. Light function may return earlier, while full-load activity usually needs phased progression.
Following rehabilitation guidance consistently is one of the strongest predictors of durable recovery.
Prevention and lifestyle strategies
Practical prevention includes workstation ergonomics, frequent short breaks, variation of repetitive tasks, and gradual progression of physical load.
Avoiding prolonged "push-through-pain" behavior is important. Early response to recurrent symptoms often prevents escalation.
Optimizing general health and comorbidity management can improve tissue recovery and reduce recurrence risk in long-term care.
Patient action plan: what to do step by step
If symptoms are mild and recent, start with 2–3 weeks of structured load modification and avoidance of movements that clearly provoke pain. Track whether symptoms settle at rest and whether hand function improves in daily tasks. This helps distinguish temporary overload from a condition that needs formal diagnostic work-up.
If symptoms persist or repeatedly return with normal activity, the next step should be specialist assessment with focused clinical examination and selected imaging when indicated. At this stage, the key objective is precise diagnosis and a treatment pathway aligned with your functional goals (work capacity, sport return, and daily hand use).
If red flags develop—progressive weakness, persistent night pain, worsening range of motion, or clear decline in hand performance—do not delay review. Earlier reassessment usually reduces treatment complexity and lowers the risk of long-term functional deficit.
More about the author's research and teaching is on the Publications & training page.
Read also
- Carpal Tunnel Syndrome: Symptoms, Diagnosis, and Treatment | Guide | Artur Soczka, MD, PhD

- Trigger Finger: Conservative vs Surgical Treatment | Guide | Artur Soczka, MD, PhD
- Tennis Elbow: Lateral Elbow Pain and Treatment | Guide | Artur Soczka, MD, PhD
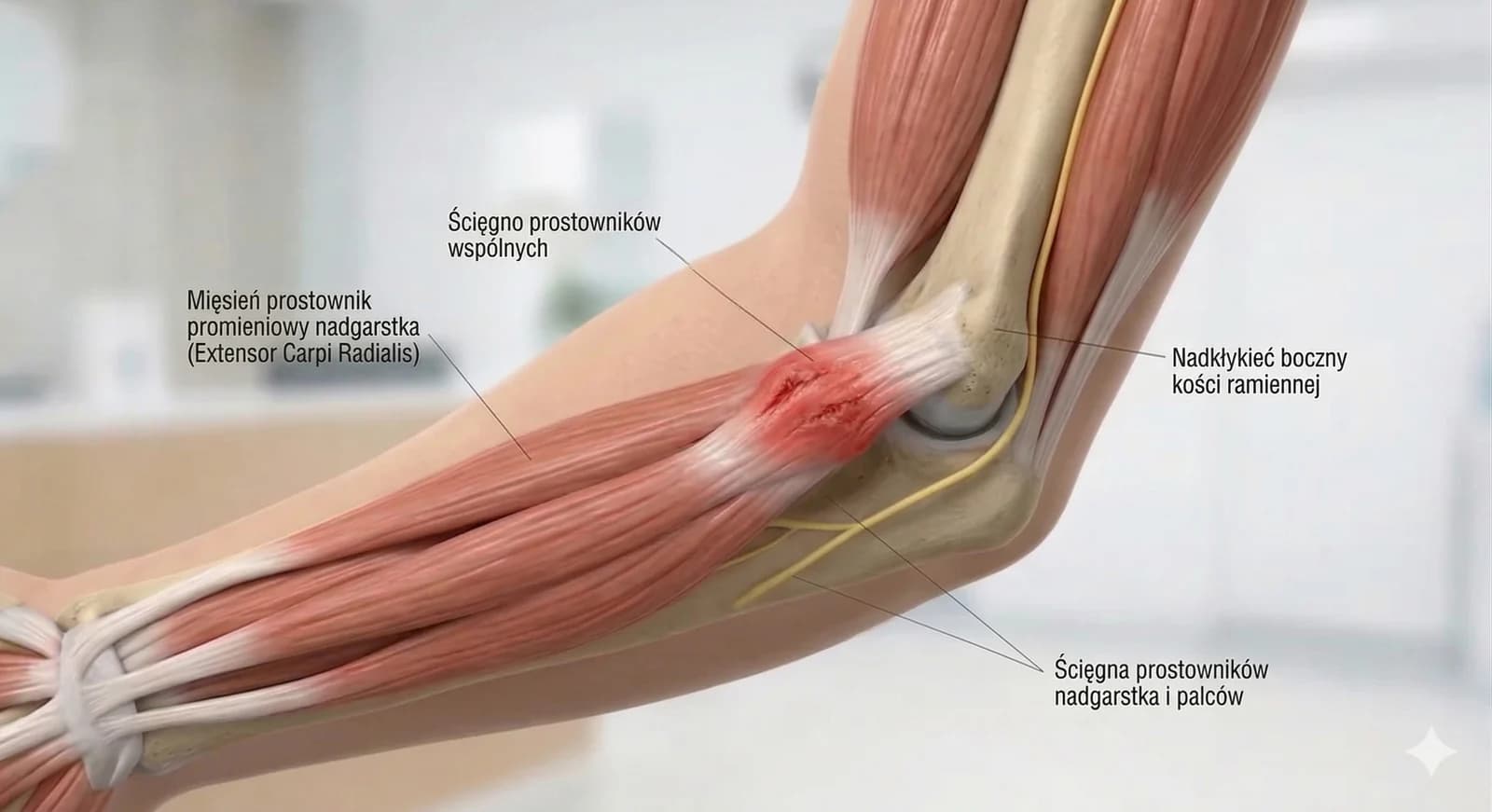
- Golfer's Elbow: Medial Elbow Pain and Therapy | Guide | Artur Soczka, MD, PhD
